9 September 2015:

Some of the 4th year students and KarenBeth at Mulago Hospital prior to going up to the patient units.
Today I helped to precept the 4th Year Pharmacy Students during their experiential learning time at Mulago National Referral Hospital. It has been a regular part of the BPharm curriculum to have the students go to the hospital to find patients who have the diseases that they are studying in class and “work them up” so they can present the information to their class members and faculty at the weekly case presentations. Before I became involved with clinical teaching at Makerere, the students didn’t have any guidance or any faculty facilitating this learning experience. The students were not always quite sure what information to gather and if they found any drug therapy problems, this wouldn’t be discussed until the case presentations, which was likely to be too late to help the patient. Last year as part of the new PCSL, I developed a “precepted” experience at the hospital so that students could have guidance about what information to collect and ask the patient about and also to be able to identify problems that could be solved that day and communicated to the physicians.
The other pharmacists helping to precept the students today were Cathy, the Makerere faculty member who came to the USA to study with me this summer, Patrick, one of the first pharmacists that came to the USA to study with me, and Winnie, a pharmacist I met back in 2012 who has since achieved a Masters of Clinical Pharmacy degree from South Africa (SA). Wow, what a difference this is since I was first practicing at Mulago in 2012. And I’m thrilled to have objective evidence that the skills the Ugandan Pharmacists learned while working with me at my hospital in Pennsylvania, are not only being put to use to help patients but also are being taught to students. I’m also very happy that Winnie, recently back from SA with her degree is able to use her skills and knowledge as a volunteer to help teach the Makerere pharmacy students in the clinical setting.
Every time I work at Mulago Hospital, it seems there is no lack of issues to be uncovered and today was no different. One of the student groups was able to identify that a patient who was a known diabetic had not been started on his diabetes medicine in the hospital and since he had an infection, it is very important to keep his blood sugar under control for proper healing. The way they found this out is simply because they asked the patient if he had carried any past medical records to the hospital with him. I have learned from my past experiences that patients are responsible for keeping their own medical records so that when they go to different doctors and clinics, they can bring the records with them. It is interesting that these records are handwritten in a small blue book, very similar to the “blue books” that are used for University examinations (small books for writing essays). I’m not faulting the medical intern who initially saw the patient because there may be a host of reasons he didn’t gain access to the old record including being extremely busy taking care of many patients at a time or perhaps the patient was drowsy or unable to communicate. But helping with issues such as this is only one way a pharmacist can be a critical member of the healthcare team. While we focus on the medication issues that are our area of expertise, the physician and nurse can focus on their areas. Then together we can collaborate to be sure all pertinent information is considered when treatment decisions are made.
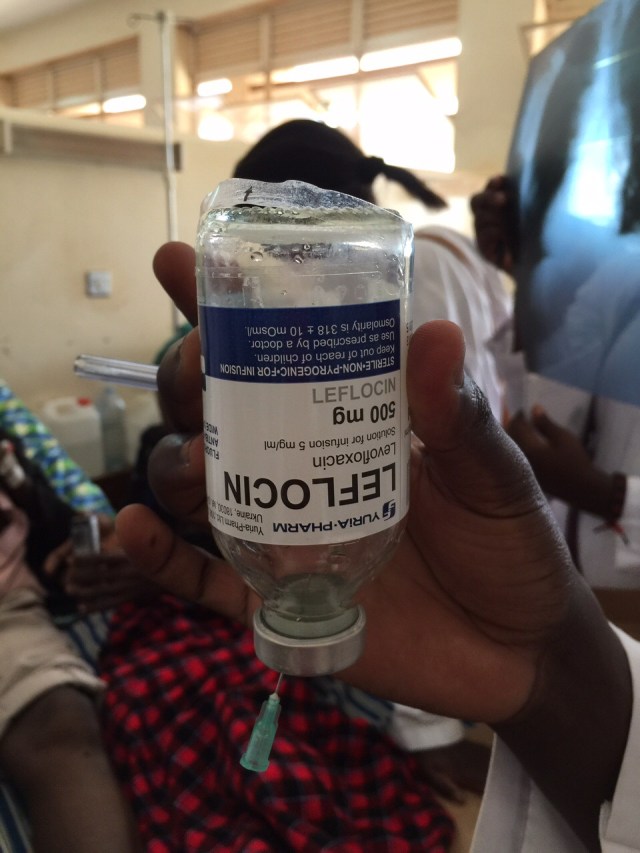
One of the patient’s caregivers wasn’t able to tell us if the antibiotic had been given to the patient. She kept telling us that only fluids were given. But when we were able to find a vial of the antibiotic and show it to the caregiver, she recognized it and was able to confirm that a similar vial had been administered. By the way, this drug, levofloxacin, is commonly used in the USA, too. This is one way pharmacists can help with the medications.
One of my ideas for further work in Uganda is to develop an Interprofessional Team of pharmacy students, medical students and nursing students from the USA and bring them to work with the same disciplines here at Mulago Hospital. This type of learning experience is becoming very important in the USA right now and most of the healthcare professions have required that their teaching programs include experiences where students of different professions and learn while working together with patients. This is called Interprofessional Education (IPE). When fully licensed practitioners work together it is called Interprofessional Practice (IPP). I think this model of care could really help manage the patient load at Mulago Hospital and result in better patient health outcomes.

This is an image of the courtyard in one part of the extremely large Mulago Hospital. You can see how the caregivers gather here to dry laundry and cook food.
Another one of the pharmacy student groups today recognized that a patient had been ordered some labs (they call them “investigations” here) but the blood was never drawn for the tests. Two of the student spent some time trying to track down someone to accomplish this task. It turned out there were a couple of reasons they weren’t done. First of all, the lab ran out of test tubes so the patient’s caregiver had to go to a pharmacy and purchase 2 vials for the blood. Even once the tubes were available, it turns out that no medical student had been assigned to take care of him, and apparently this is the person who is supposed to do the lab-work. So, this patient was caught in a “catch-22”. Only the medical student will draw the blood but no medical student was attached to this patient. This, unfortunately, isn’t a rare problem. There are quite a few “system” issues that need to be addressed and remedied in addition to enhanced healthcare practitioner education, before overall patient care can be improved. Sometimes it is easy to get discouraged and think that that things will never get better, but one must be patient and have persistence. I have seen many positive improvements since I first started working in Uganda. Of course, there is more work to be done but there are two common idioms I like to use to keep me and the students thinking positively. First, “Dream BIG but take small steps, and second, “2 steps forward, 1 step back is still forward progress.”


Nice work
LikeLike